 Printer-friendly PDF file
Printer-friendly PDF fileJune 22, 2021
Can You Trust a Public Health Department That Lies?
An Epic Lie: $167.4 Million Database That Couldn't
 Printer-friendly PDF file
Printer-friendly PDF file
June 22, 2021
Can You Trust a Public Health Department That Lies?
An Epic Lie: $167.4 Million Database That Couldn't
by Patrick Monette-Shaw
“Help, I lost my patient!”
I first heard that plaintive cry from a Certified Nursing Assistant (CNA) running up and down stairs and hallways when I worked at Laguna Honda Hospital (LHH) for a decade. She couldn’t find a patient she was supposed to be monitoring as a “sitter” using 1:1 observation.1
The sight of the distressed CNA would have bordered on being comical, had it not involved patient safety. Luckily, the patient was eventually found safe. But had the outcome been different, the nurse would have been in a lot of trouble and may have faced discipline for failing to provide 1:1 patient monitoring she had been assigned to.
 But what if “Help, I lost my patient!” turned out to apply to an entire Public Health Department that claimed it couldn’t track patients who had been discharged out of county from its hospitals?
But what if “Help, I lost my patient!” turned out to apply to an entire Public Health Department that claimed it couldn’t track patients who had been discharged out of county from its hospitals?
Imagine that the San Francisco Department of Public Health (SFDPH) had initially obtained Board of Supervisors budget approval for a $341.9 million overhaul of its electronic health record (EHR) system for patients of its public hospitals and clinics network. The $341.9 million was offset by $161.6 million in savings by eliminating existing contracts and other operating costs, for a revised project total of $181.3 million. (Funding for the replacement EHR was later reduced to needing just $167.4 million.)
Then imagine the same Department asserted after the new EHR was rolled out and implemented when it went live almost two years earlier in August 2019, that the new system doesn’t track whether patients were discharged out of county.
That claim was complete hooey! But it’s remarkably like losing your patient and unable to do post-discharge follow-up.
 DPH’s History of Lying
DPH’s History of Lying
I began a quest for out-of-county discharge data after badgering the Laguna Honda Hospital Joint Conference Committee (LHH-JCC) — a subcommittee of the San Francisco Health Commission — for months during 2012 and 2013 to publicly release aggregate data on the number of LHH patients discharged out of county. The then-chairperson of the LHH-JCC was Health Commissioner David Sanchez, who finally agreed during the LHH-JCC’s November 21, 2013 meeting that LHH would begin reporting out-of-county discharge data beginning in January 2014, mid-year into FY 2013–2014.
 The first trickle of data I obtained was for 28 LHH patients discharged out of county during FY 2013–2014. SFDPH even produced out-of-county discharge data for LHH patients going back to July 1, 2006 and continued providing me with periodic updates of out-of-county discharge data during the past eight years. As of the date of this article, San Francisco hospitals have discharged at least 1,746 San Franciscans out-of-county, but the data is wildly incomplete for several reasons.
The first trickle of data I obtained was for 28 LHH patients discharged out of county during FY 2013–2014. SFDPH even produced out-of-county discharge data for LHH patients going back to July 1, 2006 and continued providing me with periodic updates of out-of-county discharge data during the past eight years. As of the date of this article, San Francisco hospitals have discharged at least 1,746 San Franciscans out-of-county, but the data is wildly incomplete for several reasons.
 On January 3, 2020 I placed a records request to SFDPH seeking data on out-of-county discharges from SFGH and LHH between July 1, 2019 and December 31, 2019. After several months of being stonewalled due to COVID, I persisted by placing numerous follow-up requests. SFDPH finally claimed on September 16, 2020 that its recently replaced electronic health records (EHR) system named “Epic”:
On January 3, 2020 I placed a records request to SFDPH seeking data on out-of-county discharges from SFGH and LHH between July 1, 2019 and December 31, 2019. After several months of being stonewalled due to COVID, I persisted by placing numerous follow-up requests. SFDPH finally claimed on September 16, 2020 that its recently replaced electronic health records (EHR) system named “Epic”:
“… does not track OOC discharges, meaning the requested information is not readily available. Instead, the numbers must be counted manually, which will be time-consuming and involve use of scarce public resources. In addition, we are not required to create a document not already in existence. Admin. Code §67.21(1).”
First, DPH’s claim that it is not required to create documents not in existence was patently ridiculous, because California Government Code §6253.9(a)(2) — which is part of the California Public Records Act (CPRA) — specifically requires local agencies to extract aggregate data from databases they maintain. It was even more ridiculous because DPH had been extracting data on out-of-county discharges for at least eight years, since 2013.
SFDPH seems incapable of understanding that extracting data from existing databases housing the records is not the same thing as creating new records.
 Second, it turns out that Epic, the new EHR system, does in fact track discharge destinations. SFDPH had lied, however unintentionally.
Second, it turns out that Epic, the new EHR system, does in fact track discharge destinations. SFDPH had lied, however unintentionally.
I continued questioning DPH’s public records staff, asking whether SFGH was continuing to use another database known as SFGetCare that dates back to 2006, which I strongly believe captures out-of-county discharge information. Despite the public records staff having asked SFGH repeatedly whether it was still using SFGetCare, they apparently never received a clear answer from SFGH.
When I pushed DPH’s public records staff again on May 4, 2021 for discharge data for two more different time periods (between 7/1/20 and 12/31/20, and between 1/1/21 and 4/30/21) DPH again responded on May 19, 2021:
“DPH’s electronic records system does not currently track out of county discharges.”
 This is complete nonsense, and more than likely a lie (however inadvertent). If that were true, then the $100 million to $167 million budgeted would make Epic the database that couldn’t — the polar opposite of The Little Engine That Could.
This is complete nonsense, and more than likely a lie (however inadvertent). If that were true, then the $100 million to $167 million budgeted would make Epic the database that couldn’t — the polar opposite of The Little Engine That Could.
SFDPH’s wild assertion that its new Epic database does not track patients who have been discharged out-of-county is not the first time DPH has been caught lying.
Back on May 29, 2014 DPH’s then- and current-Transitions Manager, Kelly Hiramoto, claimed to then-Supervisor David Campos during a Board of Supervisors hearing that DPH had no way of ascertaining out-of-county discharge data because “a database had not worked as designed.” DPH’s then-Director of Public Health, Barbara Garcia, who was present during that hearing, didn’t correct Hiramoto’s falsehood for Campos.
 Subsequently, DPH’s then-Public Information Officer, Nancy Sarieh, claimed in response to one of my records requests on June 9, 2014 that the database that “had not worked as designed” was the SFGetCare database. I knew then Sarieh’s claim was complete nonsense, because the SFGetCare database had been rapidly prototyped from a database I had helped develop for over a decade while an employee at LHH that I knew damn well had contained discharge destination tracking.
Subsequently, DPH’s then-Public Information Officer, Nancy Sarieh, claimed in response to one of my records requests on June 9, 2014 that the database that “had not worked as designed” was the SFGetCare database. I knew then Sarieh’s claim was complete nonsense, because the SFGetCare database had been rapidly prototyped from a database I had helped develop for over a decade while an employee at LHH that I knew damn well had contained discharge destination tracking.
As I wrote four years ago in December 2017, I was concerned seven years ago in 2014 about the risk of reputational harm to RTZ Associates so I e-mailed RTZ’s owner, Rick Zawadski, on June 20, 2014 seeking a request for comment on Sarieh’s claim the SFGetCare database didn’t work as designed. He replied on June 23, saying:
“RTZ Associates stands behind the functionality and integrity of the software we have developed for the City of San Francisco, and any data fields related to LHH Diversions requested by the City of San Francisco are fully functional and work as designed.”
 Zawadski was being diplomatic in countering Hiramoto’s and Sarieh’s misinformation — their lie.
Zawadski was being diplomatic in countering Hiramoto’s and Sarieh’s misinformation — their lie.
Why would SFDPH and San Francisco’s Department of Aging and Adult Services (DAAS) collaboratively spend over $13 million across an almost 20-year period (between 2003 and 2021) for many enhancements to the functionality of SFGetCare, including adding additional new modules? Why would anyone continue to pay for something that didn’t work?
 That Hiramoto and Sarieh were able to lie is due, in part, to the fact that City employees testifying during Board of Supervisors hearings are not required to do so under oath, or under the penalty of perjury; they can — and do — lie during official Board meetings. [That may be why disgraced public officials like Mohammed Nuru, the former head of the Department of Public Works, get away with corruption.] And sadly, there’s no requirement in San Francisco’s Sunshine Ordinance or in CPRA that public records staff in each City department abstain from lying. They’re not under oath, either.
That Hiramoto and Sarieh were able to lie is due, in part, to the fact that City employees testifying during Board of Supervisors hearings are not required to do so under oath, or under the penalty of perjury; they can — and do — lie during official Board meetings. [That may be why disgraced public officials like Mohammed Nuru, the former head of the Department of Public Works, get away with corruption.] And sadly, there’s no requirement in San Francisco’s Sunshine Ordinance or in CPRA that public records staff in each City department abstain from lying. They’re not under oath, either.
 Of interest, the fifth amendment to RTZ’s contract indicated DPH intends to migrate functionality of several SFGetCare modules into DPH’s EHR system purchased from Epic.
Of interest, the fifth amendment to RTZ’s contract indicated DPH intends to migrate functionality of several SFGetCare modules into DPH’s EHR system purchased from Epic.
SFDPH may also have cast reputational harm — however inadvertently — when it claimed Epic Corporation’s EHR system doesn’t track patients who are discharged out-of-county.
The Long, Winding Road to Epic’s Intergalactic Headquarters
 You have to love a corporation that appears to have a sense of humor. Epic Systems Corporation’s website reports its Intergalactic Headquarters is located at 1979 Milky Way in Verona, WI — about nine miles southwest of Madison, WI. Epic has nine international offices, including in Saudi Arabia; the United Kingdom; Denmark; The Netherlands; Finland; Dubai, UAE; Melbourne, Australia; and Singapore.
You have to love a corporation that appears to have a sense of humor. Epic Systems Corporation’s website reports its Intergalactic Headquarters is located at 1979 Milky Way in Verona, WI — about nine miles southwest of Madison, WI. Epic has nine international offices, including in Saudi Arabia; the United Kingdom; Denmark; The Netherlands; Finland; Dubai, UAE; Melbourne, Australia; and Singapore.
Epic lists no offices on planets other than on Earth, and there are no intergalactic offices listed anywhere within the Milky Way Galaxy, or anywhere between the Milky Way, the Triangulum Galaxy, the Canis Major Dwarf Galaxy, the Sagittarius Dwarf Elliptical Galaxy, or the Andromeda Galaxy. We’ll have to see how soon Epic grows into a truly intergalactic corporation. Meanwhile, Epic Corporation’s sense of humor is at least refreshing, albeit hyperbolic.
 That said, Epic was founded with one-and-a-half employees in a basement in 1979. Forty-one years later, Epic has grown into an employee-owned corporation having 10,000 employees as of 2019. Its revenue has grown to $2.9 billion as of 2018 (ostensibly annual revenue) from its academic medical centers, community hospitals, city governments, and other clients. In San Francisco, Epic’s clients include the San Francisco Department of Public Health, UCSF, Sutter Health (including CPMC facilities), Kaiser Permanente Hospital, and Brown and Toland Physician Services — each of whom appear to be using Epic’s MyHealth internet portal for patients to communicate with their doctors and hospitals.
That said, Epic was founded with one-and-a-half employees in a basement in 1979. Forty-one years later, Epic has grown into an employee-owned corporation having 10,000 employees as of 2019. Its revenue has grown to $2.9 billion as of 2018 (ostensibly annual revenue) from its academic medical centers, community hospitals, city governments, and other clients. In San Francisco, Epic’s clients include the San Francisco Department of Public Health, UCSF, Sutter Health (including CPMC facilities), Kaiser Permanente Hospital, and Brown and Toland Physician Services — each of whom appear to be using Epic’s MyHealth internet portal for patients to communicate with their doctors and hospitals.
SFDPH’s Road to Epic’s Intergalactic HQ
Since 2010, SFDPH had relied on its Invision / Lifetime Clinical Record (LCR) system from Siemens Medical Solutions USA, Inc. (acquired by Cerner Corporation in 2015), for DPH’s electronic medical records system that had been in use for over 20 years. DPH faced risking or losing a substantial portion of its $650 million annual revenue from Medi-Cal (Medicaid), Medicare, and commercial insurance companies unless it consolidated multiple legacy computer systems, many outdated, into a single platform to unify EHR systems between hospitals and clinics. Cerner did not plan to support DPH’s EHR systems after the year 2020.
 SFDPH began its trek down the road to Epic’s intergalactic headquarters in 2016.
SFDPH began its trek down the road to Epic’s intergalactic headquarters in 2016.
Beginning with investments made in the FY 2015–2016 budget under then-Mayor Ed Lee, SFDPH began laying the foundation for its new enterprise-wide EHR. In early 2016, the Board of Supervisors authorized then Director of Public Health Barbara Garcia to enter into negotiations with UCSF Medical Center for shared use of UCSF’s existing EHR, called Advanced Patient Centered Excellence (APeX). After two years of planning and infrastructure preparation, DPH began negotiating sharing use of APeX as the Health Commission’s and DPH’s top departmental priority. DPH’s goal was to begin implementation in FY 2016–2017.
In 2016 the Board of Supervisors authorized DPH to negotiate directly with the Regents of UCSF for shared use of UCSF’s EHR system that had evolved from APeX into a potential sublicensing accreditation agreement between UCSF and Epic Systems Corporation, because UCSF had become an Epic “Community Connect” partner.
 After negotiating with UCSF for six months but unable to reach a fair and reasonable agreement for both entities, DPH began a competitive solicitation program to procure its own EHR system. Eventually, Epic City Government, LLC — a wholly-owned subsidiary of Epic Systems Corporation — was awarded a ten-year contract term with SFDPH for $167.4 million, including a $17.9 million contingency amount, with an option to extend the contract for one or more terms.
After negotiating with UCSF for six months but unable to reach a fair and reasonable agreement for both entities, DPH began a competitive solicitation program to procure its own EHR system. Eventually, Epic City Government, LLC — a wholly-owned subsidiary of Epic Systems Corporation — was awarded a ten-year contract term with SFDPH for $167.4 million, including a $17.9 million contingency amount, with an option to extend the contract for one or more terms.
The contract involved installing and hosting Epic, along with migrating and archiving data from DPH’s previous EHR system into Epic.
To date, vendor payments in the City’s DataSF database shows that almost $93 million has been spent, or is in the remaining balance, for Epic’s purchase and implementation.
Table 1: Epic Vendor Payments FY 17–18 to FY 20–21
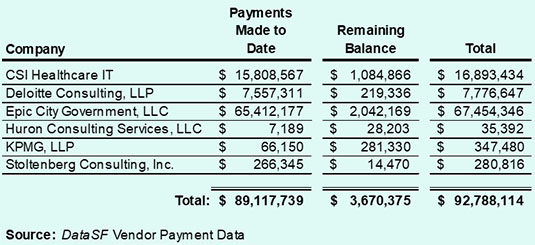
 Of the $89.1 million spent to date, $65.4 million (73.4%) has been paid to Epic City Government. It’s not yet known whether the $23.7 million paid to date to vendors other than to Epic is in addition to the $167.4 million contract with Epic, or if the $23.7 million is coming from additional sources of funding. The ongoing operating costs and annual fees to Epic for maintenance and hosting are estimated by the Board of Supervisors Budget and Legislative Analyst (Harvey Rose’s LLC) to be $20 million.
Of the $89.1 million spent to date, $65.4 million (73.4%) has been paid to Epic City Government. It’s not yet known whether the $23.7 million paid to date to vendors other than to Epic is in addition to the $167.4 million contract with Epic, or if the $23.7 million is coming from additional sources of funding. The ongoing operating costs and annual fees to Epic for maintenance and hosting are estimated by the Board of Supervisors Budget and Legislative Analyst (Harvey Rose’s LLC) to be $20 million.
SFDPH issued a press release on August 20, 2019 indicating that its Epic electronic health record system went live with its August 3 Wave 1 launch, presumably after the migrating and archiving of data from its previous EHR system into Epic had been completed. The Wave 1 launch involved DPH’s largest patient care facilities at SFGH, LHH, primary care and specialty outpatient clinics, and numerous ancillary service programs. An infographic shows Wave 2 involves other ancillary services (including Jail Health Services) that appear to mostly have gone live during 2020; DPH says it may be still rolling out portions of Wave 2. Planning for unknown features yet to be rolled out during Wave 3 is apparently just beginning.
 The infographic indicates SFDPH rolled out a “whole person care” module named “Coordinated Care Management” in the third quarter of calendar year 2020 during Wave 2 implementation. The module supports programs for people with intellectual and developmental disabilities, mental health challenges, and other social barriers.
The infographic indicates SFDPH rolled out a “whole person care” module named “Coordinated Care Management” in the third quarter of calendar year 2020 during Wave 2 implementation. The module supports programs for people with intellectual and developmental disabilities, mental health challenges, and other social barriers.
DPH has not responded yet to a records request asking whether SFDPH may have purchased an additional and optional Epic add-on module known as “Clinical Case Management” (CCM), and if it did when it may have been rolled out. One of the primary features of the CCM module includes additional Discharge Placement tools case managers and discharge planners can use to track the discharge destinations being considered for any given patient and which destination is ultimately chosen.
 Epic HQ Refutes SFDPH’s Nonsense (Lie)
Epic HQ Refutes SFDPH’s Nonsense (Lie)
Epic’s web site describes Epic and its EHR features, indicating the standard, base “enterprise” Epic package includes a “Patient Flow” module is included; it’s a standard component, not an add-on. The Patient Flow module includes a “LOS Reduction” feature with discharge management tools for discharge planners and members of interdisciplinary care teams. LOS refers to length-of-stay reduction to help shorten patient stays in acute care hospitals.
 After consulting with its in-house subject-matter experts, Epic’s Media Relations Department confirmed that the Patient Flow application includes database fields for Discharge Disposition — the broad category of where a patient is discharged to, e.g., returned to home vs. discharged to a skilled nursing facility, a rehabilitation facility, a Long-Term Care Acute Hospital (LTCAH), or perhaps a Residential Care Facility for the Elderly (RCFE) — and the actual discharge location (including the name, address and City, phone number, and type of facility).
After consulting with its in-house subject-matter experts, Epic’s Media Relations Department confirmed that the Patient Flow application includes database fields for Discharge Disposition — the broad category of where a patient is discharged to, e.g., returned to home vs. discharged to a skilled nursing facility, a rehabilitation facility, a Long-Term Care Acute Hospital (LTCAH), or perhaps a Residential Care Facility for the Elderly (RCFE) — and the actual discharge location (including the name, address and City, phone number, and type of facility).
Epic’s Media Relations department indicated Epic also has an optional “Clinical Case Management” add-on module with primary features for Discharge Placement that case managers can use to track which discharge destinations were considered and which location was ultimately chosen.
Epic’s Media Relations staff also indicated that in addition to standard reporting tools, information systems computer professionals can write their own custom, facility-specific, ad-hoc database queries into Epic’s various components, including its Patient Flow, LOS Reduction, or Clinical Case Management modules.
 According to the City Controller’s payroll database for the period ending June 30, 2020 SFDPH had 156 Information Systems employees on its staff, collectively paid $20.7 million, including 46 “I.S. Engineers,” 102 “I.S. Business Analysts,” and 8 “I.S. Programmer Analysts.”
According to the City Controller’s payroll database for the period ending June 30, 2020 SFDPH had 156 Information Systems employees on its staff, collectively paid $20.7 million, including 46 “I.S. Engineers,” 102 “I.S. Business Analysts,” and 8 “I.S. Programmer Analysts.”
Surely at least one of those 156 DPH employees should know computer programming well enough to be able to write a simple ad hoc database query in Epic (and store it for subsequent re-use) to extract aggregate data on how many patients have been discharged out-of-county.
After all, during my decade assisting with developing a Microsoft Access relational database at LHH, I learned that a selection of records combination query is as easy to write as “Like San Francisco” against a patient’s address and city at the time of admission, plus “Not Like San Francisco” against the patient’s address and city at the time of discharge … even if the two data points are stored in separate tables within the same database.
 That data selection combination would obviously identify only San Franciscans who were discharged out-of-county, precisely because San Francisco is the only city in San Francisco County. Ergo: any patient not discharged to an address in San Francisco automatically was an out-of-county discharge. The simple query logic to identify which data to extract is obvious, even to me in spite of my not being a computer programmer.
That data selection combination would obviously identify only San Franciscans who were discharged out-of-county, precisely because San Francisco is the only city in San Francisco County. Ergo: any patient not discharged to an address in San Francisco automatically was an out-of-county discharge. The simple query logic to identify which data to extract is obvious, even to me in spite of my not being a computer programmer.
Since Epic’s subject matter experts double-checked and confirmed that the discharge destination data is a standard feature incorporated into Epic’s base enterprise system, having to write such a database query would only be required if Epic doesn’t already include such a built-in “canned” report in its library of standard reports.
Following the patient sexual abuse scandal at LHH announced in June 2019, its disgraced CEO, Mivic Hirose, was let go but her golden parachute landed her a cushy $230,464 annual salary job as an Informatics Clinical Nurse Specialist in SFDPH’s Information Technology unit assisting the Clinical Informatics team with configuring, testing, implementing and training clinical staff on aspects of Epic’s EHR package. Hirose’s resume showed she has no formal training or on- the-job experience in computer science, information systems, or informatics. Perhaps that’s why SFDPH falsely claimed Epic doesn’t track out-of-county discharges.
the-job experience in computer science, information systems, or informatics. Perhaps that’s why SFDPH falsely claimed Epic doesn’t track out-of-county discharges.
My own healthcare clinician contacts and my primary care physician — whose group practice is affiliated with Brown and Toland, an Epic client — have confirmed discharge disposition data is available in Epic’s core enterprise package, secondary confirmation SFDPH’s claim Epic doesn’t track out-of-county discharges is a lie, when not pure hooey.
SFDPH brags on its COVID-19 data web page that San Francisco’s “response to the coronavirus emergency is grounded in data, science and facts,” and claims DPH is “committed to providing accurate, reliable reports to the public.”
 If DPH really believes in providing accurate and reliable facts to the public, how can you trust this public health department about COVID or anything else, when it lies about whether its $167.4 million EHR database is able to track how many of its patients have been discharged out-of-county?
If DPH really believes in providing accurate and reliable facts to the public, how can you trust this public health department about COVID or anything else, when it lies about whether its $167.4 million EHR database is able to track how many of its patients have been discharged out-of-county?
Since Epic verified its EHR system does, in fact, capture discharge destinations by the city each patient is discharged to, SFDPH should immediately comply with California Government Code §6253.9(a)(2) and extract the aggregate out-of-county discharge data I had requested.
Monette-Shaw is a columnist for San Francisco’s Westside Observer newspaper, and a member of the California First Amendment Coalition (FAC) and the ACLU. He operates stopLHHdownsize.com. Contact him at monette-shaw@westsideobserver.com.
1 1:1 observation is used to provide safety to patients who may be suffering from cognitive impairment, may be at risk of falling, or who may cause harm to themselves or others. It requires keeping a patient within sight at all times of the day and night.