 Printer-friendly PDF file
Printer-friendly PDF fileMarch 31, 2023
A Secondary Analysis of LHH’s “Root Cause” Problems
Pre-Mortem of a Hospital:
One-Year Anniversary
Preliminary Analysis of Quantitative Root Factors Is Scary and
Refute Claims Diminishing Severity of LHH’s Violations
by Patrick Monette-Shaw
[Note: I ask for readers’ indulgence with this necessarily long article meant to help preserve the historical record of LHH’s mismanagement.]
April 14, 2023 is the one-year anniversary of LHH’s decertification.
It’s taken two months to wade through reading, digesting, and reflecting on the two root causes analysis reports Laguna Honda Hospital (LHH) commissioned to uncover the underlying factors that led to LHH’s decertification from the Medicare Program, along with other documents released on February 8. Background material for this article total 669 pages, hence this in-depth article.
LHH’s residents deserve to have this history told. And read. And preserved. They deserve to be cared for safely.
 It was shocking to learn the 63 detailed root causes uncovered now requiring 454 corrective actions to resolve 138 citations LHH has received. LHH had violated 78 separate patient care-related “F-Tags” — many multiple times each — plus an additional 20 “K-Tag” violations of facility “physical plant” deficiencies across the three years and four months since the sexual abuse of patients scandal at LHH surfaced in 2019. The 98 various types of “Tag” deficiencies led to the 138 citations.
It was shocking to learn the 63 detailed root causes uncovered now requiring 454 corrective actions to resolve 138 citations LHH has received. LHH had violated 78 separate patient care-related “F-Tags” — many multiple times each — plus an additional 20 “K-Tag” violations of facility “physical plant” deficiencies across the three years and four months since the sexual abuse of patients scandal at LHH surfaced in 2019. The 98 various types of “Tag” deficiencies led to the 138 citations.
The sheer volume of the 138 citations involving the 78 F-Tag violations was even more shocking to the cadre of dedicated current employees and alumni who served at LHH over the years. They are mostly not responsible for the current sad situation at LHH and will suffer from the negative publicity. They are people who feel proud of their work providing LHH’s residents with high levels of care.
 The alumni don’t have to be present at LHH today to surmise origins of these citations. Most of them remain shocked because citations before had never been so severe, with so many violations of basic patient care regulations.
The alumni don’t have to be present at LHH today to surmise origins of these citations. Most of them remain shocked because citations before had never been so severe, with so many violations of basic patient care regulations.
It was only when interloping managers from SFGH and the San Francisco Health Network (SFHN) began running LHH in the past three years like it was an acute care hospital instead of as a skilled nursing facility that the citations mushroomed. The inept managers are principally responsible for the current mess at LHH, not LHH’s caring and dedicated staff.
Even more shocking are attempts by San Francisco City officials, including the Board of Supervisors, who have baldly tried desperately to diminish the scope and severity of the 138 deficiencies and citations, and the causal factors that led to them.
To dispel attempts to falsely diminish the severity of LHH’s patient care violations, consider a few numbers.
One-hundred and thirty-eight. One-hundred and twenty-three. Two-hundred and sixty-one.
Those may not sound like very large numbers, but 138 is the shocking number of actual substandard patient care violations plus facility physical plant citations Laguna Honda Hospital (LHH) has racked up as a result of State survey inspectors during the three-year, four-month period following the patient sexual abuse scandal that first rocked the hospital in July 2019. That’s a lot of violations over a short period.
Add in another 123 substandard care violations uncovered during an unofficial inspection conducted by LHH’s in-house consultant, Health Management Associates (HMA), during LHH’s first “mock survey” done in June 2022 to prepare LHH for an official re-certification survey by the California Department of Public Health (CDPH). A planned second “Mock Survey” was never held, without explanation.
LHH tried to minimize the 123 “Mock Survey” findings by claiming here were only 101 unduplicated F-Tag violations, creatively excluding 22 repeated F-Tags.
 That totals 261 patient care, and facility, violations of Federal regulations, suggesting severe problems with regulatory compliance to provide quality of care safely to LHH’s vulnerable residents. All along and at every opportunity LHH, the Board of Supervisors, and City officials have minimized the severity and scope of the violations.
That totals 261 patient care, and facility, violations of Federal regulations, suggesting severe problems with regulatory compliance to provide quality of care safely to LHH’s vulnerable residents. All along and at every opportunity LHH, the Board of Supervisors, and City officials have minimized the severity and scope of the violations.
But there’s no escaping the fact that 261 problems — requiring up to 454 corrective actions identified as necessary — can’t simply be brushed off as outliers, or “minimal,” as the “minimizers” have asserted. The problems occurred primarily due to inept management brought in to LHH who had no experience whatsoever managing a skilled nursing facility.
This isn’t about LHH’s ability to walk and chew gum at the same time, as Supervisor Myrna Melgar cavalierly asserted, along with her pal, Supervisor Hillary Ronen.
LHH has been in the throes of potential closure for now a full year following its decertification on April 14, 2022 as a participating provider in the Federal government’s Centers for Medicare and Medicaid (known as Medi-Cal in California) Services (CMS) participation program for skilled nursing facilities (SNF’s).
To receive reimbursement from CMS, SNF’s must remain in substantial compliance with approximately 211 “F-Tags” required by various Federal regulations designed to protect nursing home residents, along with other regulations. LHH was found to have extensively violated those regulations during the past three years.
 It wasn’t always this way. LHH was typically in substantial compliance with CMS’ regulations and routinely passed State inspections with few, if any, regulatory violations. What is new is the recent massive mismanagement of LHH.
It wasn’t always this way. LHH was typically in substantial compliance with CMS’ regulations and routinely passed State inspections with few, if any, regulatory violations. What is new is the recent massive mismanagement of LHH.
When a trove of records were released belatedly on February 8, we began learning the severity and scope of just how serious LHH’s violations have been. The records released read like a pre-mortem of a hospital’s potential death spiral.
 Doctors Derek Kerr and Maria Rivero published a terrific article on February 23 in the Westside Observer summarizing a portion of the root causes that led to LHH’s decertification in a report San Francisco’s Department of Public Health had succeeded at keeping secret for nine weeks. Their article is a must read for anyone interested in the fate of LHH and its dwindling resident population.
Doctors Derek Kerr and Maria Rivero published a terrific article on February 23 in the Westside Observer summarizing a portion of the root causes that led to LHH’s decertification in a report San Francisco’s Department of Public Health had succeeded at keeping secret for nine weeks. Their article is a must read for anyone interested in the fate of LHH and its dwindling resident population.
Kerr and Rivero have been an investigative whistleblower and watchdog team for the Observer for approaching 20 years. [Disclosure: When Dr. Rivero served as LHH’s Medical Director, she extended my job offer when I was hired at LHH in 1999. A decade later, I helped proofread and format their seminal “Critical Analysis of the Ja Report” in 2009 about a behavioral health program proposed for LHH.]
LHH’s Institutional Comorbidities
Kerr’s and Rivero’s article in February covered the initial 48-page Root Cause Analysis (RCA) Report prepared by Health Services Advisory Group (HAG), a consultant that has been paid $17.3 million to date to assist LHH obtain re-certification from CMS. That report was released on February 8 following drawn out public records requests to obtain it.
I only take slight issue with an editor’s caption to an illustration accompanying their article that suggests the initial RCA report dated December 1, 2022 finally gives us a complete picture of LHH's problems and the path to recovery. A complete picture is premature, given there was a second 36-page RCA report describing LHH’s first “90-Day Monitoring Survey” dated January 31, 2023 and a 49-page “Action Plan” report listing 454 corrective actions needed to fix LHH’s mismanagement.
A second 90-Day Monitoring Survey that began on March 13 planned to take a week that concluded in March 17 will be followed by a third RCA report and a potential additional “Action Plan.” I’m hesitant to conclude we’ve seen a complete picture of LHH’s problems decades long in the making.
Just as individual patients often have multiple, co-existing, long-term medical conditions — known as comorbidities that may develop independently of one other but may not directly cause each other — hospitals, institutions, and skilled nursing facilities can also develop multiple long-term, systemic, and chronic conditions that threaten their survival.
Kerr and Rivero’s February Westside Observer article explored five of the first eight problem areas in the first RCA report exploring the causal root factors leading to LHH’s decertification, including:
But following the Fire Life Safety inspection resulting in four “Immediate Jeopardy” citations over a fire alarm debacle during the first 90-Day Monitoring Survey CMS and the California Department of Public Health (CDPH) conducted at LHH in December, the list of eight problem areas grew to 11, including the last three:
![]() 6. Medication Management and Administration
6. Medication Management and Administration
7. Resident Rights and Freedom from Harm
8. Emergency Preparedness Program
9. Fire and Life Safety
10. Resident Quality of Care
11. Food and Nutrition Services
The additional three problem categories outline significant problems State inspectors uncovered between December 1 and December 16 after the first 90-Day Monitoring survey wrapped up.
The final two categories, Resident Quality of Care and Food and Nutrition Services, were among the most damning, which will be reviewed in detail in an upcoming article.
 Back in May 2015, Drs. Kerr and Rivero’s Westside Observer article, “Laguna Honda’s Falling Star,” documented LHH’s CMS five-star rating plummeted to just two stars. Four years following their 2015 article, LHH’s patient sexual abuse scandal surfaced in June 2019. That was when LHH was slapped with CMS’ then new, red stop-hand warning icon for consumers. Since then, LHH sank to it’s current pathetic one-star CMS rating. The warning icon remains next to LHH’s name to this day on CMS’ Nursing Home Compare website.
Back in May 2015, Drs. Kerr and Rivero’s Westside Observer article, “Laguna Honda’s Falling Star,” documented LHH’s CMS five-star rating plummeted to just two stars. Four years following their 2015 article, LHH’s patient sexual abuse scandal surfaced in June 2019. That was when LHH was slapped with CMS’ then new, red stop-hand warning icon for consumers. Since then, LHH sank to it’s current pathetic one-star CMS rating. The warning icon remains next to LHH’s name to this day on CMS’ Nursing Home Compare website.
The 261 Citations
In the three years and four months since news reports surfaced reporting LHH’s sexual abuse scandal in July 2019, the hospital racked up 261 citations across 12 State survey inspections.
Chart 1:
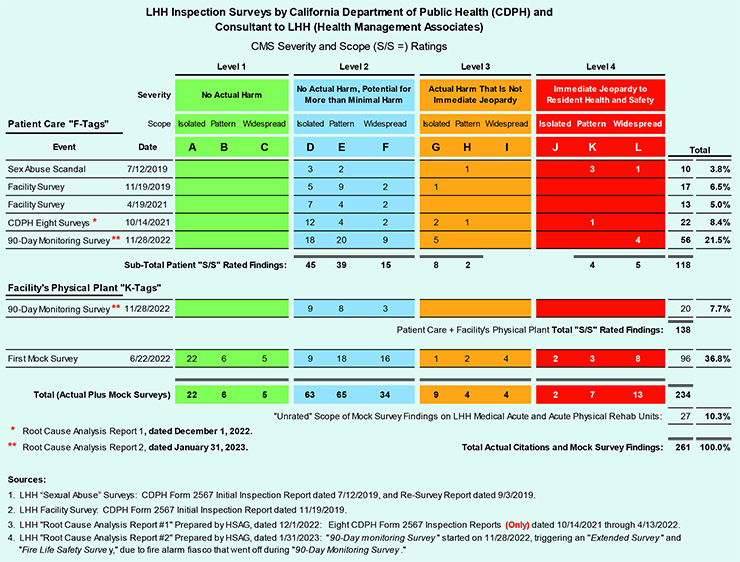
 Chart 1 shows:
Chart 1 shows:
 When the near-fatal patient fentanyl overdoes happened in July 2021, it triggered a succession of eight separate State survey inspections beginning on October 14, 2021 and running through April 13, 2022, during which LHH ignored successive CMS and CDPH warnings that it faced potential decertification for worsening violations. Across those eight successive survey’s, LHH racked up a total of 22 citations, including another citation alleging a pattern of “Immediate Jeopardy” violations, until CMS finally resorted to decertifying LHH on April 13, 2022. It is thought CMS had the option of placing LHH in receivership, but didn’t.
When the near-fatal patient fentanyl overdoes happened in July 2021, it triggered a succession of eight separate State survey inspections beginning on October 14, 2021 and running through April 13, 2022, during which LHH ignored successive CMS and CDPH warnings that it faced potential decertification for worsening violations. Across those eight successive survey’s, LHH racked up a total of 22 citations, including another citation alleging a pattern of “Immediate Jeopardy” violations, until CMS finally resorted to decertifying LHH on April 13, 2022. It is thought CMS had the option of placing LHH in receivership, but didn’t. Fast forward to LHH’s first 90-Day Monitoring Survey that began on November 28, seven months after being decertified. At that point, LHH received a whopping 56 patient-care related citation violations, plus 20 “physical plant” (facility) violations, for a total of 76 violations — representing a combined 28.8% of the 261 total citations across the actual official survey inspections and the unofficial “Mock Survey” citations.
Fast forward to LHH’s first 90-Day Monitoring Survey that began on November 28, seven months after being decertified. At that point, LHH received a whopping 56 patient-care related citation violations, plus 20 “physical plant” (facility) violations, for a total of 76 violations — representing a combined 28.8% of the 261 total citations across the actual official survey inspections and the unofficial “Mock Survey” citations.In total, LHH racked up 118 patient care citations in those intervening three years and four months. Chart 1 shows LHH also racked up 20 citations related to “physical plant” deficiencies uncovered during the first 90-Day Monitoring Survey for a total of 138 citations across the 12 formal State survey inspections.
 Toss in another 123 rated and un-rated citations uncovered during an unofficial “Mock Survey” conducted by LHH’s consultant Health Management Associates (HMA) which has been paid $5.8 million to date to assist LHH gain CMS re-certification. That brings total citations for various known LHH deficiencies to 261 — which is clearly a symptom of mismanagement of the hospital in this LHH pre-mortem.
Toss in another 123 rated and un-rated citations uncovered during an unofficial “Mock Survey” conducted by LHH’s consultant Health Management Associates (HMA) which has been paid $5.8 million to date to assist LHH gain CMS re-certification. That brings total citations for various known LHH deficiencies to 261 — which is clearly a symptom of mismanagement of the hospital in this LHH pre-mortem.
A full-page version of Chart 1 is available on-line.
Spolier Alert
Unfortunately, just before publication of this secondary analysis article, news surfaced that numbers presented here may be under-reported.
On March 21, LHH’s acting CEO, Roland Pickens, announced during a full Health Commission meeting that LHH’s second CMS/CDPH “90-Day Monitoring Survey” had concluded, apparently on Friday, March 17. He gushed that LHH had only been slapped with an additional 23 new deficiencies that he didn’t describe or summarize, and which haven’t been released to the public yet. It’s worrisome the 23 new deficiencies — a bucket of ice-cold water — may push recertification further on back, whicht is already way behind schedule.
Another records request has been placed to obtain CDPH’s new Form 2567 report rapidly, rather than having to wait for HSAG to write a third “Root Cause Analysis” report and another follow-up supplementary “Action Plan” for CMS.
 The potential 23 new citations will push LHH’s total citations since July 2019 to a new total of 284 citations, up from 261. Hopefully, LHH hasn’t received another “Immediate Jeopardy,” which it had been warned not to by CMS.
The potential 23 new citations will push LHH’s total citations since July 2019 to a new total of 284 citations, up from 261. Hopefully, LHH hasn’t received another “Immediate Jeopardy,” which it had been warned not to by CMS.
During the March 21 Commission meeting, Pickens claimed LHH had received 124 deficiencies during its first “90-Day Monitoring Survey.” He appears to have been confused, or mis-spoke, because the second “Root Cause Analysis” report documented 76 citations (50 related to patient care plus 20 “facility” citations). Pickens may have been trying to compare and contrast the new 23 deficiencies to the 76 deficiencies (but wrongly claimed 124) in an effort to claim LHH has been making progress on implementing reforms and reducing the number of citations.
But there’s no escaping the fact that if LHH just received 23 additional patient-care related deficiencies, that would still be more than the 22 citations which led to LHH’s decertification across the 8 separate inspection forms. While a reduction from 76 to 23 between two surveys is progress, 23 more citations suggests LHH still isn’t ready yet to pass an actual recertification survey!
 It’s not yet known how many additional “milestone” corrective actions will be needed in another “Action Plan” to fix the 23 new citations. It’s also not known if the new corrective milestones will also have to be corrected by May 13 along with the other 454 milestones. This portends LHH will definitely have to undergo a third “90-Day Monitoring Survey,” which probably won’t start until mid-June.
It’s not yet known how many additional “milestone” corrective actions will be needed in another “Action Plan” to fix the 23 new citations. It’s also not known if the new corrective milestones will also have to be corrected by May 13 along with the other 454 milestones. This portends LHH will definitely have to undergo a third “90-Day Monitoring Survey,” which probably won’t start until mid-June.
Attaining actual CMS recertification looks farther and farther away to the detriment of LHH’s current residents and San Franciscans needing admission to LHH but can’t get in given the continuing ban on any new admissions.
By the time LHH received the new 23 deficiencies on March 21, LHH had not updated the Health Commission about whether between November 18 and December 16 (or after) all 123 deficiencies identified in the “Mock Survey” conducted in June (that Pickens had tried to pretend were only 101 deficiencies) had been cured, since only 63 had been fully resolved with the remaining 38 unresolved by November 18. Following LHH’s dashboard report for the week ending November 18, LHH stopped presenting publicly weekly dashboard reports in December, so it’s unclear whether those 38 remaining deficiencies were ever fully resolved.
A reasonable person would assume the 38 outstanding deficiencies would have been resolved in the five months between June and November, but the status of their resolution vanished into thin air before LHH was hit with the 23 new citations.
Scope of the Citations
Across the 12 survey’s between June 2019 and April 2022 another perspective is the sheer numbers within each “scope” category. An alternative way of visualizing the 261 violations by severity and scope across all 12 inspectionsis is shown in the chart below.
Chart 2:
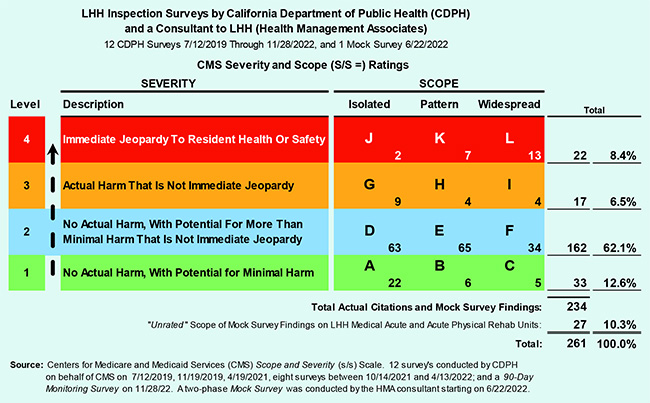
 Chart 2, also available on-line in full-page format, shows:
Chart 2, also available on-line in full-page format, shows:
 The 22 “Immediate Jeopardy” and 17 “Actual Harm” citations combined comprise 14.9% of the 261 violations.
The 22 “Immediate Jeopardy” and 17 “Actual Harm” citations combined comprise 14.9% of the 261 violations.It was beyond the resources of this article to tally the number of individual residents identified anonymously across the 12 survey inspections reports that had earned the 261 citations. But given LHH’s typical resident census was 710 people, and given the scope ranged from isolated to widespread incidents, it’s not a stretch to imagine that the aggregate number of patients affected may have neared or exceeded the 710 residents.
For instance, just one inspection — on July 12, 2019 involving the sexual abuse allegations that had earned four “Immediate Jeopardy” scope ratings of “pattern” or “widespread” — had found 21 residents had been harmed by physical, mental, verbal, and sexual abuse, and chemical and physical restraints; and 5 residents had endured life-threatening complications as a result of receiving purloined medications from LHH staff that had not been prescribed by their LHH physicians.
About the “F-Tags”
For those who may want to get into the weeds, Table 1 available on-line lists the titles of each of 78 separate “F-Tag” (patient care) violations. CMS’s is thought to have 211 separate “F-Tag” criteria all skilled nursing facilities nationwide are required to comply with; 48 of the 211 — 22.7% — involve sub-standard care, by definition.
 So, the 78 F-Tags LHH violated — accounting for 118 actual survey patient care citations and an additional’ 57 “Mock Survey” patient care F-Tags findings in the 261 citations — represents 37% of all 211 F-Tags. That suggests LHH’s widespread and potentially willful disregard of the “F-Tag” CMS standards.
So, the 78 F-Tags LHH violated — accounting for 118 actual survey patient care citations and an additional’ 57 “Mock Survey” patient care F-Tags findings in the 261 citations — represents 37% of all 211 F-Tags. That suggests LHH’s widespread and potentially willful disregard of the “F-Tag” CMS standards.
This bears repeating: The sheer volume of citations during the three years was being mismanaged as if it were an acute care hospital, not as a skilled nursing facility (SNF), is a symptom of, and result of, LHH having been run by managers having no experience in running SNF’s.
Add in 38 “K-Tag” (physical plant) violations across LHH’s actual inspection report citations plus the “Mock Survey” findings, out of an unknown number of total “K-Tags.” Again, that suggests LHH’s willful neglect to keep its “physical plant” in safe operating condition to house its vulnerable residents.
About the “Federal Regulatory Groups”
 As for “Federal Regulatory Group” categories, Table 2 also available on-line illustrates that the 118 citations LHH received for “F-Tag” patient care violations across the 12 inspections spanned 17 of 21 Regulatory Groups.. Of the 118, fully 40 — 34% — involved quality of patient care and resident-centered care plans.
As for “Federal Regulatory Group” categories, Table 2 also available on-line illustrates that the 118 citations LHH received for “F-Tag” patient care violations across the 12 inspections spanned 17 of 21 Regulatory Groups.. Of the 118, fully 40 — 34% — involved quality of patient care and resident-centered care plans.
The “Regulatory Groups” are analogous to organs and parts of the body, such as the brain (Hospital Administration), heart (Nursing Department), liver (Quality Management Department), lungs (Medical Services Department), stomach, kidneys, and skin (encompassing the “physical plant”), and eyes, arms and legs, etc. Given the scope and severity of LHH’s diseased citations, it necessitated this pre-mortem, if you will. LHH’s prognosis from the 261 citations, is poor.
If you agree the sheer quantitative numbers in this preliminary analysis of root causes leading to LHH’s decertification and its subsequent inspections are scary, the qualitative narrative in a planned next installment are even scarier.
About the Causal “Root Factors”
 Never mentioned was the need for LHH to implement a “culture of managers” qualified to run SNF’s.
Never mentioned was the need for LHH to implement a “culture of managers” qualified to run SNF’s.
Table 3 is a detailed list of the 63 underlying root causes grouped by each of the 11 major problem categories across the first two RCA reports exploring the causal root factors leading to LHH’s decertification. A sampling of some of the more shocking root causes includes:
There are other equally alarming root causes contained in Table 3 on-line.
As Kerr and Rivero rightly noted in their February 23 article that although HSAG bravely exposed many of the underlying root causes that led to LHH’s decertification, HSAG omitted mentioning in its two Root Cause Analysis reports that the disastrous “Flow Project” of SFGH patients routed to LHH beginning in 2004 as having been the start of LHH’s decline. Kerr and Rivero noted:
“The Root Cause Analysis [reports] omits [that] foundational history, but covers its grim outcome” and also observed the “[root cause analysis reports] exposes the ignorance and mismanagement that befell the hospital.”
 Sadly, none of the managers who allowed these root causes to first germinate and then flourish have been held accountable. None have been terminated to date, except LHH’s recent CEO, Michael Phillips, who served for just two years, long before the problems had begun. He was let go, but nobody else has been.
Sadly, none of the managers who allowed these root causes to first germinate and then flourish have been held accountable. None have been terminated to date, except LHH’s recent CEO, Michael Phillips, who served for just two years, long before the problems had begun. He was let go, but nobody else has been.
A Word on Methodology
Data presented in the two charts and four tables in this pre-mortem include a divergence in reporting. The first “Root Cause Analysis” HSAG had been contracted to produce under it’s $2.6 million contract to be LHH’s Quality Improvement Expert (QIE) — and it’s additional $14.7 million in consulting contracts to steer LHH toward recertification — was supposed to have been based on analyzing the “root causal factors” behind the 22 citations contained in the eight CDPH on-site inspection Form 2567 reports CDPH conducted between October 14, 2021 and April 13, 2022.
But when the first Root Cause Analysis (RCA) report delivered to CMS by HSAG as LHH’s QIE on December 1 was finally released to members of the public on February 8 due, in part, to the Westside Observer “Sunshine Guy’s” persistence, there were odd discrepancies.
 As shown in Table 4 also available on-line, of the 22 F-Tag citations CDPH had issued across the eight inspection survey Form 2567’s (that were to comprise the first RCA report), HSAG excluded reporting 6 of the F-Tags, and added 10 other F-Tag titles, including two involving Pharmacy Services deficiencies not listed in the initial eight Form 2567 reports. RCA #1 also asserted there had only been 21 citations, not the 22 listed on the original eight Form 2567 inspection reports. (Weirdly, the RCA reported actually listed 24 separate F-Tag deficiencies by name, not 21 and not 22.)
As shown in Table 4 also available on-line, of the 22 F-Tag citations CDPH had issued across the eight inspection survey Form 2567’s (that were to comprise the first RCA report), HSAG excluded reporting 6 of the F-Tags, and added 10 other F-Tag titles, including two involving Pharmacy Services deficiencies not listed in the initial eight Form 2567 reports. RCA #1 also asserted there had only been 21 citations, not the 22 listed on the original eight Form 2567 inspection reports. (Weirdly, the RCA reported actually listed 24 separate F-Tag deficiencies by name, not 21 and not 22.)
The first RCA report specifically stated:
“The RCA specifically addressed deficiencies identified during surveys between October 14, 2021, and April 13, 2022, and all deficiencies that were discovered and disclosed to LHH by the California Department of Public Health (CDPH), CMS, or a contract surveyor after those surveys.”
SFDPH refused the Westside Observer’s specific records request to ask the author of the first RCA report about their methodology and sources of data, and refused to provide their e-mail address. One issue was that there appeared to have been a typo in the second RCA Report dated January 31, 2023.
HSAG had claimed that during the first 90-Day Monitoring Survey that had triggered an “Extended Survey” and a “Fire Life Safety” survey all conducted in December, State inspection surveyors had identified only 66 deficiencies. In actuality, the surveyors had identified 76, not 66, citations. The Westside Observer wanted to learn what the discrepancy of 10 deficiencies might have involved.
Another question of interest to the Observer had been what other sources of deficiencies had been identified and disclosed to LHH by other contract surveyors in addition to the eight Form 2567 reports conducted by CDPH surveyors between October 2021 and April 2022. If HSAG had indeed obtained other survey reports, those sources have not yet been disclosed to members of the press or members of the public, and weren’t listed in HSAG’s first “Root Cause Analysis” report.
As well, HSAG had claimed only 62 of the 66 (or 76) deficiencies had been rated as a scope and severity of “D” or higher. In actuality, all 76 had received ratings of “D” or higher.
On closer examination, it turned out 76 separate deficiencies had in fact had been cited, but 13 of the individual patient care “F-Tags” had been cited as having multiple, duplicated instances, including one F-Tag cited three separate times, for a total of 14 duplicated F-Tags. That artificially reduced the 76 deficiencies, allowing HSAG to wrongly assert only 62 unduplicated deficiency F-Tag titles.
It was a bald attempt by HSAG to try it’s own propaganda spin control of “minimizing” the severity of problems at LHH by confounding 76 as being only 62.
A generic records request to HSAG’s headquarters for the author’s e-mail address to pose questions went unanswered. So much for SFDPH’s and HSAG’s transparency and accountability.
The Tome of Documents
Here’s some more numbers to digest:
Three-hundred and forty-seven. One-hundred and seventy-seven. Six-hundred and sixty-nine.
These numbers refer to the cookie-crumb trail of the problems described in government public records leading up to, and following, LHH’s decertification in April 2022.
The 347 number refers to the total pages in California Department of Public Health (CDPH) survey inspection Form 2567 reports following 11 separate LHH inspections between July 12, 2019 and April 13, 2022 resulting in LHH’s decertification. I’ve read all 347 pages.
 The 177 number refers to the total pages across the two Root Cause Analysis reports prepared by Health Services Advisory Group (HSAG) prepared as LHH’s contracted “Quality Improvement Expert,” Health Management Associates (HMA) initial “Preliminary Assessment” of LHH, LHH’s “Action Plan also prepared by HSAG, and the two-phase “Mock Survey” reports HMA produced. A planned second Mock Survey was scuttled, without an explanation of why.
The 177 number refers to the total pages across the two Root Cause Analysis reports prepared by Health Services Advisory Group (HSAG) prepared as LHH’s contracted “Quality Improvement Expert,” Health Management Associates (HMA) initial “Preliminary Assessment” of LHH, LHH’s “Action Plan also prepared by HSAG, and the two-phase “Mock Survey” reports HMA produced. A planned second Mock Survey was scuttled, without an explanation of why.
Add in 84 pages of CDPH penalty reports involving the 12 patient deaths post-discharge, and another 61 pages between the LHH Settlement Agreement and the initial LHH Closure Plan, and you arrive at the 669 pages of background materials. I’ve read all 669 pages.
Incomplete “60-Day Reform Plan”: LHH’s Quality Management Program
 Following the 2019 sex abuse scandal, SFDPH released a “60-day Laguna Honda Reform Plan,” claiming that as part of its Plan of Correction to CMS and CDPH, it would appoint a permanent CEO to replace LHH’s then CEO, Mivic Hirose. A year passed before an interim CEO, Maggie Rykowski, was replaced by Michael Phillips, who was hired, in part, due to his experience running an acute-care hospital and a behavioral health facility, not a skilled nursing facility. He lasted just two years and was let go in June 2022 just after LHH was LHH was decertified. So much for a “permanent” CEO.
Following the 2019 sex abuse scandal, SFDPH released a “60-day Laguna Honda Reform Plan,” claiming that as part of its Plan of Correction to CMS and CDPH, it would appoint a permanent CEO to replace LHH’s then CEO, Mivic Hirose. A year passed before an interim CEO, Maggie Rykowski, was replaced by Michael Phillips, who was hired, in part, due to his experience running an acute-care hospital and a behavioral health facility, not a skilled nursing facility. He lasted just two years and was let go in June 2022 just after LHH was LHH was decertified. So much for a “permanent” CEO.
As a reminder, because LHH had failed to report the sexual abuse incidents in a timely manner — or at all — to the California Department of Public Health (CDPH), LHH received four “Immediate Jeopardy” citations. The scandal has cost at least $1,829,212 to date in fines, penalties, and lawsuit settlements. Costs of that scandal continue to rise.
As an overarching goal, the Reform Plan claimed:
“There is more to reform LHH than just coming into compliance with regulatory findings. The goal for LHH is to build a best-in-class long-term care residential facility worthy of the patients and the people of San Francisco.”
 Unfortunately, SFDPH and SFHN kept operating LHH under Phillips as if it were an acute-care hospital, not as a skilled nursing facility, despite the claim “reform” in 2019 would get LHH to a best-in-class skilled nursing facility “place” and restore a “culture of [patient] safety” at LHH that Hirose had wantonly abandoned.
Unfortunately, SFDPH and SFHN kept operating LHH under Phillips as if it were an acute-care hospital, not as a skilled nursing facility, despite the claim “reform” in 2019 would get LHH to a best-in-class skilled nursing facility “place” and restore a “culture of [patient] safety” at LHH that Hirose had wantonly abandoned.
After the patient sexual abuse scandal rocked LHH in 2019 at a cost of $1.83 million, had the 60-Day Reform Plan actually been implemented, it may have prevented LHH’s decertification in 2022 that has already racked up $27.4 million in expenses (and continue growing) to try to get LHH back into some semblance of being a best-in-class skilled nursing facility.
The 60-Day Reform Plan written in August 2019 by the San Francisco Health Network’s (SFHN) Chief of Quality Officer, Troy Williams, asserted SFDPH was re-organizing LHH’s Quality Management Department, and would appoint a permanent Quality Management Director to ensure resident safety at LHH. Dr. Grant Colfax, Director of Public Health in San Francisco’s Department of Public Health helped develop LHH’s “Reform Plan.”
It took until June 2020 before Williams appointed Nawzaneen Talai as an interim Chief Quality Officer at LHH. She was promoted from within. Talai reports directly to Williams, not to LHH’s acting CEO, Roland Pickens.
Despite the Quality Management re-organization in 2019, quality improvement problems persisted. As Kerr and Rivero reported in February, the first Root Cause Analysis report submitted to CMS on December 1, 2022 acknowledged in Root Cause #1 of the Quality Assurance category:
“[LHH’s quality improvement] structure is designed to align with LHH’s affiliated acute care hospital within the San Francisco Network and acute care processes … [it’s] not tailored toward the SNF setting … [increasing] the risk … necessary care to residents related to SNF regulations is not delivered.”
Root Cause #3 found:
“Direct-care staff … do not contribute to daily quality improvement] activities … [resulting] in a culture of silence and indifference, increasing the likelihood that quality concerns are not raised and addressed … [placing] residents at risk for harm.”
There’s HSAG’s admission of Hirose’s “culture of silence” — a hangover from her reign of terror before being ousted — before Colfax and Williams thought up LHH’s “60-Day Reform Plan” to replace silence with a “culture of safety” Hirose had admitted she ignored.
As Kerr and Rivero reported, the first RCA report Analysis also acknowledged:
“The four new hires in the QM Department do not have SNF or healthcare quality experience, a common hiring practice throughout LHH. This gap in nursing home knowledge and experience contributes to the staff not being properly qualified or competent.”
“The four new hires in the QM Department do not have SNF or healthcare quality experience, a common hiring practice throughout LHH. This gap in nursing home knowledge and experience contributes to the staff not being properly qualified or competent.”
 These root cause findings in 2022 were a damning indictment Williams and Colfax failed to reform LHH’s QM problems in their 60-Day Reform Plan in 2019. And it took until the first RCA report to get an acknowledgement of what LHH advocates have long claimed: That the mismanagement of LHH for the past 18 years was a direct result of staff and managers who lack SNF experience. That seems to be continuing despite the first RCA report, given the hiring in March 2023 of yet another interim LHH “Chief Medical Officer” who also lacks SNF experience.
These root cause findings in 2022 were a damning indictment Williams and Colfax failed to reform LHH’s QM problems in their 60-Day Reform Plan in 2019. And it took until the first RCA report to get an acknowledgement of what LHH advocates have long claimed: That the mismanagement of LHH for the past 18 years was a direct result of staff and managers who lack SNF experience. That seems to be continuing despite the first RCA report, given the hiring in March 2023 of yet another interim LHH “Chief Medical Officer” who also lacks SNF experience.
The sex abuse citations Plan of Correction in 2019 claimed LHH would develop a new protocol to screen residents when returning from a pass to prevent the bringing of illicit substances into the facility. Whether that policy was developed, or implemented is doubtful, because the illicit substances proliferated and contributed to LHH’s decertification in April 2022.
Troy Williams’ Reform Plan claimed it would develop a Request for Proposal (RFP) to partner with healthcare consultant(s) experienced in long-term care facilities to align the care of LHH patients with the skilled nursing facility “industry” best practices. It’s not known whether the RFP was completed or whether a consultant with experience in long-term care facilities was ever hired. It’s thought the three consultants LHH eventually hired and brought on board at a current cost of $26.7 million weren’t hired until May 2022, after LHH was decertified in April 2022.
The Reform Plan asserted LHH would pursue a long-term goal of applying for Joint Commission on Accreditation of Healthcare Organizations (JCAHO), or another relevant accreditation body. LHH has never held, and thought doesn’t need to hold, JCAHO accreditation. Skilled nursing facilities (SNF) require licensure, not accreditation. This illustrates Mr. Williams was totally unfamiliar with SNF settings. It’s but one symptom illustrating SFHN and SFDPH managers were mismanaging LHH like it was an acute-care hospital, not as a SNF. Perhaps the claim was meant to portray LHH as taking a semblance of meaningful action.
No action seemed to have followed, and LHH doesn’t seem to have applied for JCAHO accreditation, or we might have heard about it by now. We haven’t.
The “Minimizers”
 Because many people keep trying to minimize the severity and scope of violations at LHH — including the Health Commission, LHH CEO Roland Pickens, Director of Public Health Grant Colfax, Supervisor Myrna Melgar, Supervisor Hillary Ronen, former City Attorney Louise Renne, and others, including even some of LHH’s community supporters — a large dose of skepticism is in order.
Because many people keep trying to minimize the severity and scope of violations at LHH — including the Health Commission, LHH CEO Roland Pickens, Director of Public Health Grant Colfax, Supervisor Myrna Melgar, Supervisor Hillary Ronen, former City Attorney Louise Renne, and others, including even some of LHH’s community supporters — a large dose of skepticism is in order.
How these “minimizers” can collectively ignore 138 State survey inspection citations, 78 “F-Tag” and “K-Tag” specific statutory violations (many multiple times systemically), 63 causal root factors, and 454 corrective actions necessary to hopefully bring LHH back into regulatory compliance to obtain recertification — is a mystery only a spin control meister, or a mother, can appreciate and love.
After all, LHH’s “Action Plan” released on February 8 listing 454 corrective action milestones is shockingly full describing basic problems in many departments at LHH.
Supervisor Myrna Melgar
Supervisor Melgar was interviewed for an inaugural San Francisco Chronicle podcast titled “Soup With the Supes” on February 28, 2023. The podcast series featuring additional District Supervisors is part of a Chronicle series titled “SF Next: Fixing Our City.
The February podcast was moderated by Chronicle multimedia journalist Laura Wenus, who opened the segment with Melgar saying the hospital was found to be “out of compliance” with regulations in April 2022, and alluded to a CDPH inspection survey in October 2021 that had revealed two patients had overdosed on street drugs in July 2021 and were discharged to acute care hospitals immediately, which saved their lives. One of them had to be placed in a breathing machine. Wenus blithely said only that Federal regulators had found “LHH was in a state of substandard quality of care.” In truth, LHH had been routinely and repeatedly out of substantial compliance with regulations for at least three years.
It’s clear Wenus hadn’t read the 64-page October 14, 2021 CDPH Form 2567 inspection report. That inspection had not only revealed the two life-threatening fentanyl overdoes, but that 13 of 37 sampled residents had tested positive for illicit street drugs, two patients had been found unconscious, and two had sustained falls. Also, 23 of the 37 sampled residents were found to have contraband articles that posed a safety hazard jeopardizing the health and safety of other residents, with 11 of the 37 deemed unsafe smokers possessing ignitable items having the potential to cause burn injuries and significant harm to residents. Other serious deficiencies were also noted during the October survey, which were only the beginning of causal factors following seven subsequent inspections leading to LHH’s decertification in April 2022.
 The October 2021 inspection wasn’t merely about two patient overdoes, as Wenus glossed over.
The October 2021 inspection wasn’t merely about two patient overdoes, as Wenus glossed over.
For her part, Melgar said she had “been working my butt off for Laguna Honda since the beginning” [of becoming District 7 Supervisor], in part “because the things they [CMS] were asking us to do were against our best interests, against the best interests of the residents of Laguna Honda. The Relocation Plan was a total disaster.”
Melgar was referring specifically to LHH’s initial “Closure Plan” (LHH Closure and Patient Transfer and Relocation Plan) that CMS required LHH to adopt and implement. Weirdly, CMS tied it to LHH’s concurrent efforts to obtain re-certification.
Melgar was right the ill-conceived Closure Plan was a disaster and against the best interests of LHH’s residents, because it had led to 12 patient deaths post-discharge among the first 57 involuntary transfers and discharges.
Melgar went on to recount how she helped mobilize community opposition to the Closure Plan. She said, “It was indicative of our working together and use whatever assets we had to deal with the ‘political problems’ while we were also dealing with the ‘technical issues’ with CMS.” Calling resolving the Closure Plan a “political” problem was strange, but alluding to the serious substandard quality of care violations as mere “technical” problems was even weirder, minimizing the severity and scope of LHHS’ problems CMS had uncovered.
Melgar admittedly was instrumental in passing two resolutions at the Board of Supervisor urging Secretary of the US. Department of Health and Human Services, Xavier Becerra, to get CMS and CDPH to agree to a pause on the patient transfers.
 Beyond the Closure Plan, which was admittedly wrong to have required, what Melgar missed or tried to minimize and gloss over was that CMS was principally asking that LHH — as DHHS Secretary Xavier Becerra subsequently rightfully noted — fix all of the substandard care and 261 deficiencies that led to LHH’s decertification and return to being in substantial compliance with all 211 “F-Tag” patient care standards.
Beyond the Closure Plan, which was admittedly wrong to have required, what Melgar missed or tried to minimize and gloss over was that CMS was principally asking that LHH — as DHHS Secretary Xavier Becerra subsequently rightfully noted — fix all of the substandard care and 261 deficiencies that led to LHH’s decertification and return to being in substantial compliance with all 211 “F-Tag” patient care standards.
That, ultimately, is in the best interests of LHH’s residents, as Melgar and Ronen must know. To suggest not doing so is what would be against residents’ best interests, and ridiculous or Orwellian speak.
In a Chronicle article ten days earlier on February 18 about a delayed affordable housing project for LHH’s campus that will include market-rate housing to help fund the affordable housing tiny studio apartments planned for the campus, Melgar was quoted as saying“We should be able to walk and chew gum at the same time,” saying she felt “caught between a rock [obtaining LHH’s recertification] and a hard place” [the housing project]. She was frustrated other SFDPH staff hasn’t been deployed to help shoehorn the housing in as another high priority.
“We need to save the hospital. That’s the No. 1 priority,” she said, not wanting to do anything to jeopardize recertification.
Considering LHH’s residents are caught between a rock and a hard place — mandatory involuntary discharges from LHH vs. not enduring transfer trauma and death — it’s difficult pondering sympathy for a City Supervisor feeling caught between a rock and a hard place.
Until LHH relearns how to walk, resumes full compliance with Federal regulations governing skilled nursing facilities, and regains its certification, the hospital — and by extension, SFDPH — shouldn’t even try to chew gum at the same time, let alone whine about rocks and hard places.
Supervisor Hillary Ronen
 Somewhat shockingly, Ronen seems to be casting blame and aspersions on Secretary Becerra, rather than finding fault with the very managers transplanted from SFGH and SFHN who brought LHH’s decertification on, themselves. Ronen is misdirecting blame.
Somewhat shockingly, Ronen seems to be casting blame and aspersions on Secretary Becerra, rather than finding fault with the very managers transplanted from SFGH and SFHN who brought LHH’s decertification on, themselves. Ronen is misdirecting blame.
As the San Francisco Standard reported on February 10, Ronen threw a tantrum and tweeted she was boycotting attending an SFGH Foundation gala — over her annoyance Becerra had been featured at a different City Hall event. She misplaced blame on Becerra, frothing on Twitter “[because] of his role in the deaths of 12 patients that his agency forced out of Laguna Honda Hospital & for preventing admissions [to LHH].” Becerra had no direct, or even indirect, role in the patient’s deaths. LHH did.
Ronen doesn’t seem to get it that although CMS, under Becerra, had required LHH develop a patient relocation plan — that was eventually suspended six months ago last July — it was actually LHH’s staff who were found to have been culpable for the 12 patients’ deaths, as I reported for the Westside Observer in January.
The Standard reported Ronen’s rationale for boycotting the Foundation’s gala, which was honoring Nancy Pelosi, not Becerra, was that San Francisco “shouldn’t be featuring this man at any event … when he has peoples’ lives he’s playing with.” It’s not Becerra playing with patients’ lives. That would be LHH’s own staff. More misplaced angst on Ronen’s part. Her boycott was silly. Period. It’s LHH’s managers who are playing with residents’ lives.
 This suggests Ronen may not have read any of the 261 substandard patient care citations LHH has racked up over the three years and four months between July 2019 and November 2022, or facility violations, of Federal regulations documenting severe problems with regulatory compliance to provide quality and safe care of LHH’s vulnerable residents.
This suggests Ronen may not have read any of the 261 substandard patient care citations LHH has racked up over the three years and four months between July 2019 and November 2022, or facility violations, of Federal regulations documenting severe problems with regulatory compliance to provide quality and safe care of LHH’s vulnerable residents.
It’s also unclear whether Ronen understood any of the 63 root causal factors leading to LHH’s decertification due to LHH’s mismanagement. That’s not on Becerra. He can’t simply order CMS to stop enforcing “F-Tag” violations, as she may wish.
The Standard’s article also reported Ronen asserted Becerra is:
“ … gumming up our entire system. … We’ve been bending over backwards to address any criticism they [CMS] have. … He holds us hostage every minute.”
She went on to claim LHH’s problems are “a direct result of Becerra’s failure to lead.” Ronen clearly hasn’t read my articles on LHH’s own leadership failures. Ronen has her head in the sand, or clouds.
 Ronen’s hysteria is worrisome, as if she doesn’t get it that had LHH not been providing substandard quality of care during the past three years, LHH would not need to bend over backwards now to fix 261 violations.
Ronen’s hysteria is worrisome, as if she doesn’t get it that had LHH not been providing substandard quality of care during the past three years, LHH would not need to bend over backwards now to fix 261 violations.
More worrisome, Ronen doesn’t appear to be actively opening her ears and listening to Becerra, who accurately noted:
“We are, by law, required to make sure that patients are cared for safely and with the care that they're supposed to have. … We have no choice by law but to say that the safety of patients must come first. We have to make sure that we’re all working together to make sure … everyone is following the rules [and] people are getting the care they need.”
Not content finishing bashing Becerra, Ronnen was reported in a San Francisco Chronicle article two weeks later as having written to the SFGH Foundation, saying:
“Instead of offering to assist the city, Becerra and his employees have done everything to threaten and punish Laguna Honda, and by extension, its patients.”
 Becerra hasn’t threatened or punished LHH or its patients. Instead, he’s trying to get CMS to bring LHH into compliance with CMS regulations. CMS could have put LHH into receivership, which may have gotten LHH back into compliance faster than the now year-long effort LHH has struggled with trying to obtain recertification.
Becerra hasn’t threatened or punished LHH or its patients. Instead, he’s trying to get CMS to bring LHH into compliance with CMS regulations. CMS could have put LHH into receivership, which may have gotten LHH back into compliance faster than the now year-long effort LHH has struggled with trying to obtain recertification.
Ronen doesn’t seem to get it that had LHH’s own employees not been found to have violated 78 of CMS’s 211 separate F-Tag patient care “rules” — some several times each — LHH wouldn’t have received the 118 severity-and-scope patient care citations. And Becerra and CMS would not now have to make damn sure LHH is following the rules, and the City would not have had to spend $26.7 million hiring consultants to teach LHH staff how to follow those rules.
Had Ronen read the 454 corrective action milestones listed in LHH’s 49-page “Action Plan,” she might have understood just how far out of compliance LHH had become, rather than wrongly going after Becerra.
 Even more worrisome, Ronen shouldn’t expect Becerra to simply order CMS to stop trying to get LHH back into substantial compliance. That’s what CMS is supposed to do. CMS isn’t simply punishing LHH, as Ronen wrongly presumed.
Even more worrisome, Ronen shouldn’t expect Becerra to simply order CMS to stop trying to get LHH back into substantial compliance. That’s what CMS is supposed to do. CMS isn’t simply punishing LHH, as Ronen wrongly presumed.
Hopefully, by the time the full Board of Supervisor’s holds its next scheduled Committee of the Whole hearing about LHH on May 9, Ronen may have come to her senses, and realized that it’s not Becerra who is at fault, it’s LHH’s own managers who caused LHH’s decertification.
Louise Renne, Former City Attorney and Former Supervisor
Among others who continue to minimize the severity and scope of LHH’s substandard patient care violations is Ms. Louise Renne. On March 9, 2023 the San Francisco Interfaith Council (SFIC) sponsored an “Online Briefing” for its community and faith partners featuring Renne, who shared a PowerPoint presentation titled “The Story & Fate of Laguna Honda.”
 The on-line briefing was moderated by Michael Pappas, Executive Director of SFIC, who was defrocked in 2007 as an ordained priest of the Greek Orthodox Church.
The on-line briefing was moderated by Michael Pappas, Executive Director of SFIC, who was defrocked in 2007 as an ordained priest of the Greek Orthodox Church.
Archbishop Salvatore Cordileone delivered inane remarks about saving Laguna Honda before Renne was introduced.
Renne’s slide show was ludicrous, erroneously reporting LHH’s current programming includes an active Adult Day Health Care (ADHC) program providing respite day care for elderly people who need close supervision. It doesn’t.
Renne should have known LHH’s ADHC program was shut down in 2008 even before the replacement hospital was opened in 2010 because space in the new hospital for the ADHC program wasn’t included in the rebuild floor plans. Renne should also have known LHH’s former COO, Gayling Gee, was fired by LHH’s former CEO, Mivic Hirose, for Gee’s efforts trying to save LHH’s ADHC. Renne once again wrongly claimed credit during her presentation for winning the $1 billion tobacco settlement lawsuit former Supervisor Angela Alioto had actually developed; that settlement award became part of the source of funding for the replacement hospital. As I reported in 2010, Renne had actively tried to stop Alioto’s lawsuit.
Renne claimed current City Attorney David Chiu’s had “won” his Federal lawsuit to rescue LHH. She was lying. As part of LHH’s Settlement Agreement with CMS, Chiu was forced to withdraw his lawsuit, which effectively stopped a second, separate lawsuit Renne had filed that was found to be outside the Court’s jurisdiction. Her appeal is unlikely to succeed. And she implied she’s still representing all LHH families and patients.
Chiu didn’t win anything. Instead, he surrendered by withdrawing his lawsuit. Renne must know the distinction.
Remarkably, Renne claimed LHH’s decertification was caused merely by two patients using fentanyl, other patients possessing lighters and cigarettes, and a single medication error. Nothing could be further from the truth.
She basically minimized and lied about CMS’s extensive findings and citations — and concluded by saying that saving LHH is a cause the religious faithful must take up for those who are not rich will have a place to go. She was merely inciting and stoking a public outcry. It was sad seeing her grandstanding using out-of-date information.
Asked by Pappas to expand on recent violations that led to LHH’s decertification, Renne lamely fell back on LHH’s patient sex abuse scandal in 2019. She bemoaned (like Melgar) the proposed housing project on LHH’s campus has stalled.
 Renne mentioned nothing else about more the recent and voluminous 261 State citations, or the 63 distinct root causal factors, most of which point to LHH’s inept managers. By deflecting Pappas’ question, Renne basically lied. Period.
Renne mentioned nothing else about more the recent and voluminous 261 State citations, or the 63 distinct root causal factors, most of which point to LHH’s inept managers. By deflecting Pappas’ question, Renne basically lied. Period.
Across these minimizers, I have to wonder whether any, or all, of them have read any, or all, of the 669 pages of background materials relating to LHH’s decertification. If they had, why are they minimizing the seriousness of LHH’s problems?
Of interest, the minimizers have completely avoided addressing three salient issues that they must be aware of:
Defrocking the “Minimizers”
I’m reminded of comedian and former U.S. Senator Al Franken’s 2003 book, “Lies … and the Lying Liars Who Tell Them.” Franken asserted God had suggested he title his book, “Bearers of False Witness and the False Witness That They Bear.” It was great that Franken worked with God’s suggestion, updating it to modern vernacular. His book put me on alert 20 years ago for liars.
Ironically, after the #MeToo movement arrived, Leeann Tweeden, a conservative talk-radio host, bore False Witness — lying — by alleging Franken had kissed her without her consent during a USO Tour, forcing him to resign as Senator in 2018.
I became a columnist for the Westside Observer because the truth matters, since too many people lie to attain power and abuse people. Locally, lying to us undermines our trust in SFDPH. Public figure or private, lies impose real harm.
Me? I have to keep doing my part to give voice to LHH’s voiceless.
 For those who have continued to minimize LHH’s problems, deception has been the point all along: Theatrical propaganda put out by an unreliable narrators. I have to wonder if God will defrock them for bearing False Witness, as Pappas was defrocked.
For those who have continued to minimize LHH’s problems, deception has been the point all along: Theatrical propaganda put out by an unreliable narrators. I have to wonder if God will defrock them for bearing False Witness, as Pappas was defrocked.
The minimizers need to stop their deliberate misinformation.
Sadly, LHH as we knew it may not survive it’s pre-mortem, if lies continue leading to its post-mortem.
Monette-Shaw is a columnist for San Francisco’s Westside Observer newspaper, and a retired City employee. He received a James Madison Freedom of Information Award in the “Advocacy” category from the Society of Professional Journalists–Northern California Chapter in 2012. He’s a member of the California First Amendment Coalition (FAC) and the ACLU. Contact him at monette-shaw@westsideobserver.com.